Aligner Excellence
February 23rd, 2022
Aligners are an integral tool of orthodontics. Like any tool, when handled properly, it can deliver fantastic results but unlike a hammer, not every patient is a nail. In other words, every patient is different and requires individual and unique treatment planning in order to be successful.
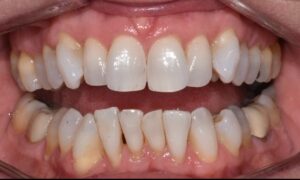
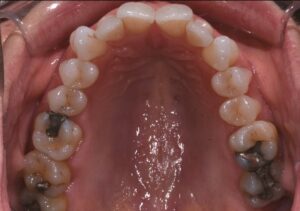
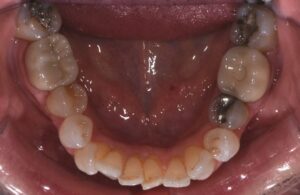
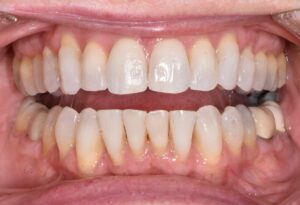
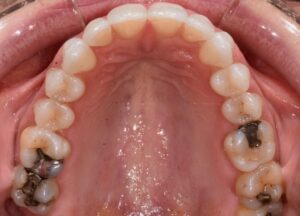
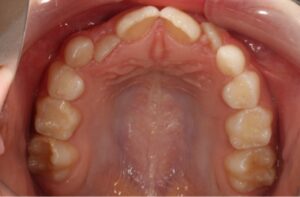
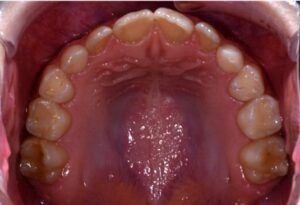
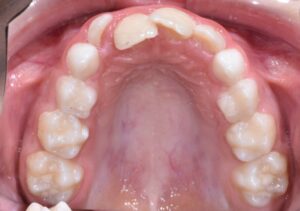
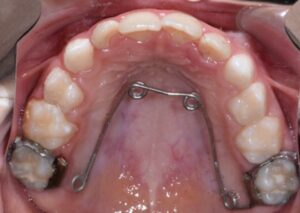
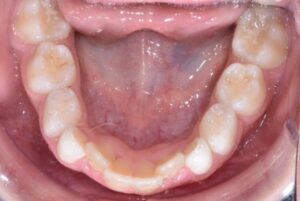
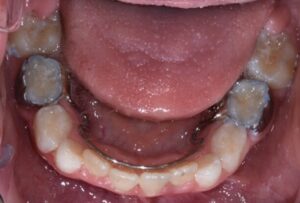
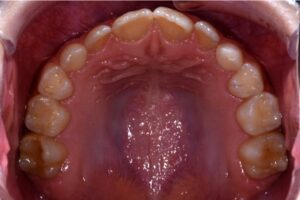
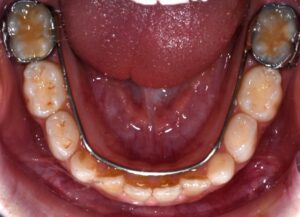
This nice lady provided an example of effective treatment planning to give her a great smile without negatively impacting her fragile gingival health. By using a combination of staged tooth movement. (i.e., moving specific teeth at specific times to avoid excessive expansion and well-designed IPR (interproximal Reduction), we were able to align her teeth for maximum health and esthetics.
IPR is where small amounts of enamel are removed from the sides of the teeth to develop space for alignment to avoid excessive expansion which can compromise the health of the gums.
Her treatment required 8 visits over 14 months
Experience and understanding of the mechanics of the tooth movement are keys to the success with any orthodontics treatment. Let us help.
Why Teeth Are Crowded?
September 9th, 2021
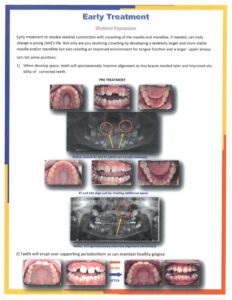
One of the most common issues we see in orthodontics is crowded teeth. Have you ever wondered why the teeth are crowded? The simple reason, besides genetics, is there is not enough space because the teeth are too big but the most often cause is the upper and the lower jaws are not big enough to accommodate the teeth. In other words, the jaws are not skeletally wide enough, if that is the case, then in most patients you would want to skeletally widen the jaws to accommodate the crowded teeth. The best time to get stabile skeletal correction with the greatest amount of ease is between 7 and 10 years old. At this age, the bones are malleable and easy to manipulate.
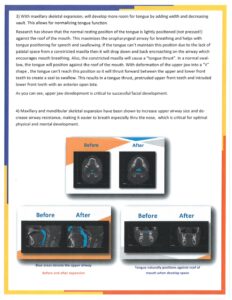
In this issue we show before and after photos of two 8 year olds. Both had the upper and lower jaws expanded. The things to notice are the width increase in the jaws and the natural alignment of the teeth which occurs spontaneously as the jaws are widened. This natural alignment creates stabile healthy teeth and gums, the process takes 8-10 months with 6 months of stabilization.
Before After
CALL TO SCHEDULE A FREE CONSULTATIONS FOR YOUR EVALUATION!
Increased Overbite (Class II)
July 7th, 2021
HOW DID WE GET HERE
The most common treatment in Orthodontics is for an increased overbite (Class II). It is also the most unpredictable because of the need for increased patient cooperation, (i.e. wearing rubber bands) the above patient had a unilateral Class II which we used braces and a TAD (Temporary Anchorage Device) to correct. The TAD takes the unpredictability out of the treatment because of the patient cooperation and the direct mechanics
Placing a TAD requires topical anesthetics. We can place one in 3 to 5 minutes. TAD’s are the way to go for predictable Class II treatment.
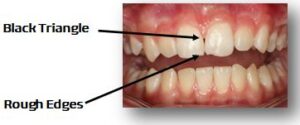
Also, we did some enamelplasty to smooth the rough edges on the upper front teeth (Centrals) and enamel reduction between these teeth to resolve the “black triangle.